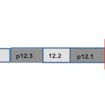
Each year, more candidate compounds for the treatment of autism spectrum disorder (ASD) are being explored. Recent findings in mouse models have particularly heightened excitement about potential treatments, with pharmaceutical interventions rescuing core behavioral, electrophysiological and molecular deficits in multiple mouse models of neurodevelopmental disease. A key discovery came from studies of a Rett syndrome mouse model — mice in which the MeCP2 gene is nonfunctional — that demonstrated that neurodevelopmental deficits can be genetically rescued even after critical developmental time windows have passed[ref]Guy J. et al. Science 315, 1143-1147 (2007) PubMed[/ref], [ref]Robinson L. et al. Brain 135, 2699-2710 (2012) PubMed[/ref]. These results give hope that individuals with neurodevelopmental disorders need not be treated very early in their time-course to gain some benefit from an effective therapy. We are, however, still missing a general understanding of what specific deficits can be rescued, and how quickly, in ASD and related neurodevelopmental disorders.